War against a virus!
An article by Dr Rajeev, a Neuroscientist from Norway published on 25/03/2020
When you hear the word ´virus´, unpleasant memories rush to your mind. It could be the painful memories of childhood chickenpox or about exhaustive viral-fever days or about scenes from Hollywood movies like Outbreak and Contagion. Not all viruses are bad though, some are beneficial to us (will discuss that topic later). These days everyone fears about the pandemic caused by a nanoscale virus called Coronavirus (CoV) that already killed several thousands and literally locked down the whole world.
This disease is named COVID-19 (COrona VIrus Disease 2019) and ´SARS CoV2´ is the virus that causes this disease. Like the ´version 2´ of the earlier SARS outbreak in 2003. SARS stands for Severe Actute Respiratory Syndrome, CoV is for Corona Virus. First, it was called the ´Wuhan virus´, then ´novel Coronavirus´ (nCoV), and still virologists are debating about its name! The similarity in the genetic sequence with the earlier SARS CoV (in the year 2003) is the reason why it is called SARS CoV2. SARS CoV2 is an RNA virus, it has approximately 30000 bases making it the largest among the known RNA viruses. The genetic material of this virus is RNA, similar to the DNA genetic material we have in our cells.
The economic loss due to COVID-19 is estimated in billions already. Only a mere percentage of that would have been sufficient to study about Coronaviruses in general (note: this is a variant of SARS CoV´1´, which broke out in 2003), including basic research on broad anti-virals, detection methods, to some extent vaccine preparations etc. We would have learned a lot about the ´Coronaviruses´ and have been easier to fight against it now! This is the situation for many diseases.
Not much about SAR2 CoV2 is known. We came to know about this around three months ago. The Scientific world is learning about its characteristics. Why is it more lethal to the elderly than young, in general? Why a vast majority gets only a mild fever, still they are silent carriers? Why some countries are the worst affected? What makes it very efficient than other Coronaviruses in transmission? How long it can stay on surfaces and in aerosols? Will it genetically drift to a more virulent one? In a matter of 3 months from the first reported case in China, it spread to almost 200 countries around the world, and the worldwide death toll crossed 18500+ (24-3-2020).
A virus is an ´infectious, obligate intracellular parasite comprising a genetic material (DNA or RNA) surrounded by a protein coat, sometimes with a membrane´ (definition by Virology Guru Prof. Vincent Racaniello @profvrr). Which means it must be inside a host cell to be functional. It depends extensively on the host cell´s machinery (hijack the cell machinery and make it into a virus reactor) to make more copies. It has a genetic material (either DNA or RNA), which carries the code to make more copies of it. Its precious genetic material is protected by a protein shell and some of the viruses like SARS CoV2 has an extra protective layer of membrane that it steals from the host cell while budding off.
Whether a virus is living organism or not, is still a debatable question. Consensus now is it has 2 phases. Phase 1, which is non-living phase outside the host cell. Phase 2, is the ´infected cell´-the virus once inside the cell overtakes the cell machineries, redirect the cell for viral replication hence the ´virus inside the infected cell´ can be considered as living.
Structure of the novel Coronavirus (SARS CoV2)
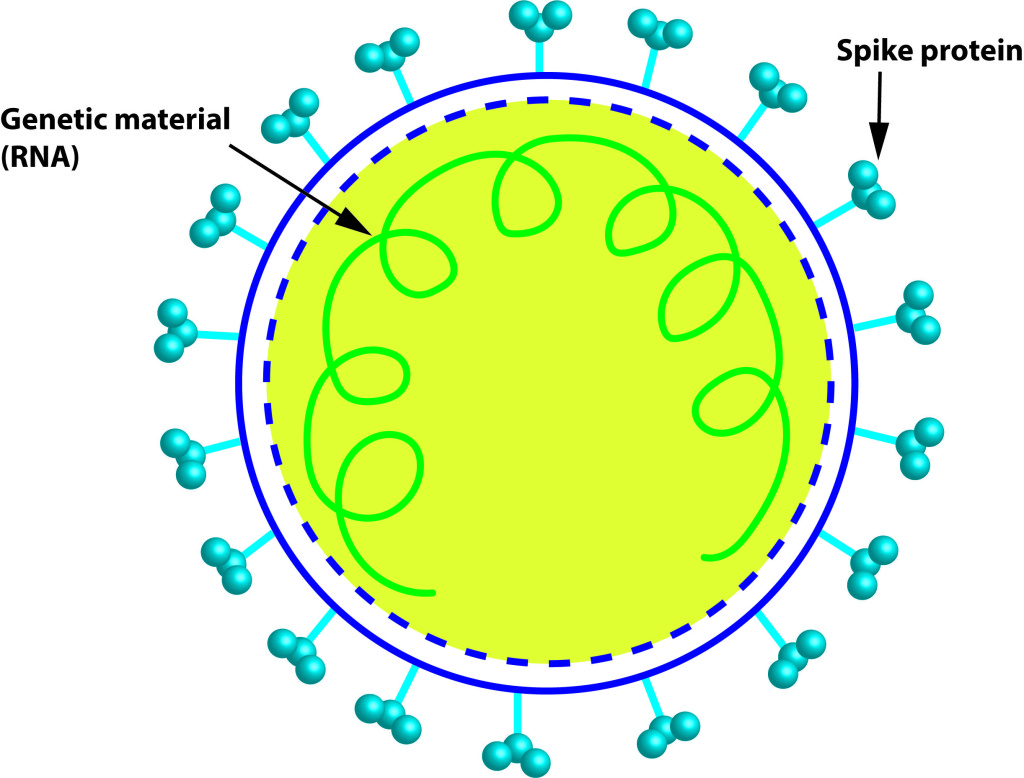
Why is the structure of a virus important to know? The protein structure is important to design drugs to fight against viruses and also to make vaccines against them. The above diagram is an oversimplified version of SARS CoV2. The spikes (they are proteins) studded on the corona (in Latin corona means a crown, also it resembles the corona of Sun) are very vital, since antibodies bind to these structures and eventually, our immune system destroys these viruses. These days, once the genomic sequence of a novel virus is revealed, one can make pieces or complete viral proteins in its proper structural conformation. Such recombined fragments or full proteins can be synthesised and purified in a research lab to use for vaccine development and also for creating antibodies against the virus. These approaches have huge potential in clinical and diagnostic applications to save millions of lives.
Cell receptors, proteases, and entry to the host cell
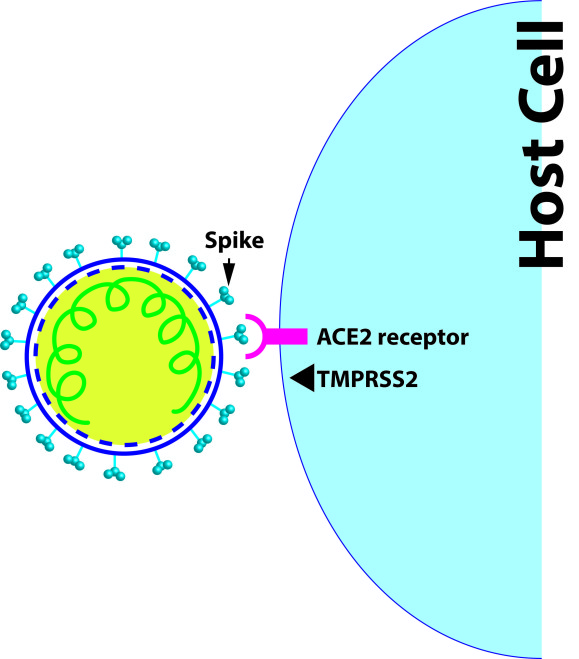
The spike proteins on the surface of this virus help to latch specifically to the host cell receptors. These receptors are identified as ACE2 receptors, note that these are cellular enzymes/proteins having dedicated functions in cell. SARS CoV2 makes use of these receptors and other cellular proteases like TMPRSS2 to release its content into the host cell. The receptors are mainly found in the respiratory tract cells, but they can be found in other vital organs of our body suggesting that they can infect those organs also. The virus utilizes ACE2 receptor to attach and subsequently with the help of cellular proteases it gets access inside the host cell. Once inside they shed its genetic material (here RNA) which will then hijack the cells machinery to make more copies of the virus. Literally making the cell it infected into a ´virus making factory´. Sometimes it takes several days for the patient to show the symptoms, that time period is called incubation period. For COVID19 it is reported as 4-14 days, while it was 2-7 days for SARS (2003 version) and 6 days for MERS. Note, you can be an infectious ´silent carrier´ during this period.
After a week, the infected person make millions of viruses mainly in lungs (which he spreads to others), forcing cells to release alarm calls which are heard by our own immune system. Which eventually destroys infected cells and cleans the battle field, resulting in recovery of nearly 80% of the infected cases. In critical cases, the destruction of the protective lining of the respiratory system opens up way to bacteria causing pneumonia and later a cytokine storm (causing deaths in COVID-19).
We need to know where the fire is!
World health organization (WHO), with their vast experience in fighting against various outbreaks, warned about the importance of ´testing´ to tame an outbreak. According to them, fighting the fire blindfolded is not efficient, we need to know where the fire is! Testing/detecting the infection is vital in an outbreak,
- to provide timely care to those infected.
- to contain the disease spreading, and protect the vulnerable.
- to understand how the disease evolves in a population.
- to lower the rate of infection and fatalities.
In the absence of timely testing, an asymptomatic ´infected person´ does not know about his/her infection hence might not quarantine, instead unknowingly go around and infect risky groups. To know the total number of people infected with COVID-19 widespread testing is warranted, unfortunately, many countries did not prepare for that. Many countries face scarcity of protective gears, testing kits, facilities, personnel for testing in the midst of this outbreak. Some countries like South Korea, Singapore were exceptional, in many places they even had drive-thru testing centers- which resulted in harnessing this outbreak to a good extent. If testing is done on ´cherry-picked´ patients, we do not have a clear picture of what’s going on. The number of ´infected´ in many countries are not the exact numbers, it is only the tip of an iceberg.
Lack of detection facilities and personnel became a nightmare at the peak of an outbreak. Which forced some research labs in countries like the USA to make their own protocols to detect this virus. Demands for testing on suspected will rise at the peak of an outbreak, and thousands of tests/day will be warranted.
How to detect COVID19 viral infection?
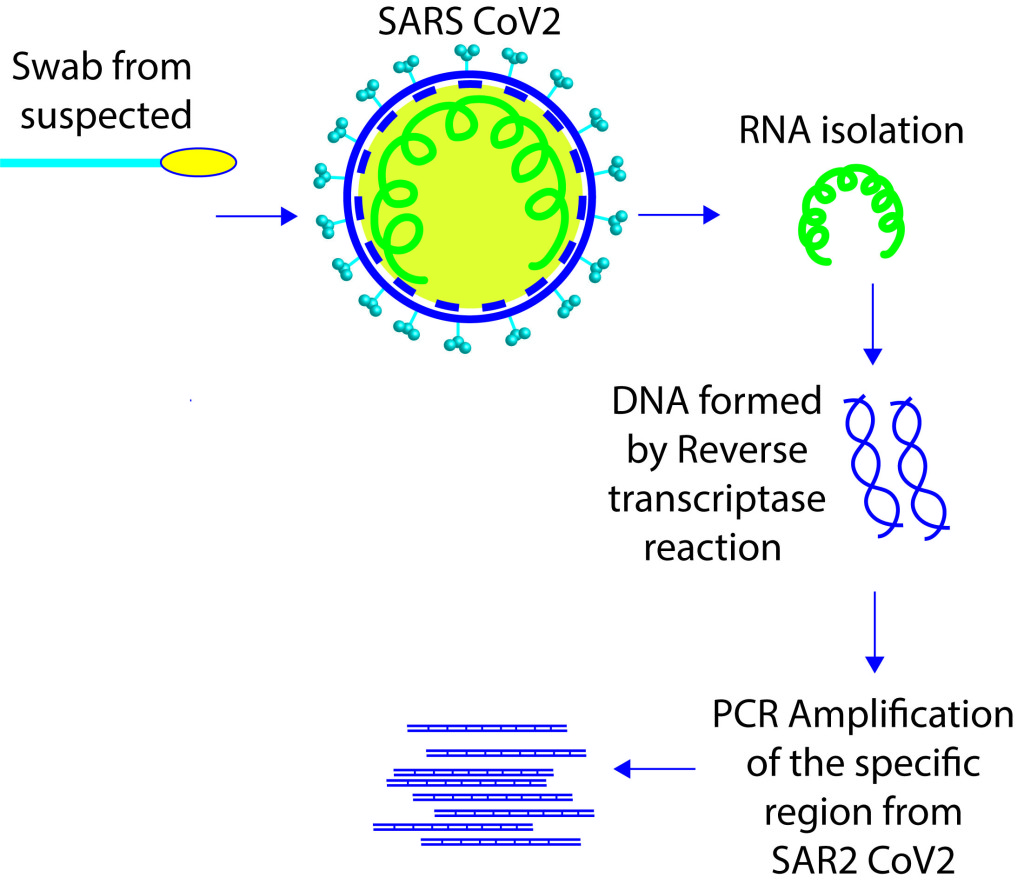
As mentioned earlier, SARS CoV2 is an RNA virus, which means the genetic material of this class of virus is a single string of ribonucleic acid (RNA). Note, we have double stranded deoxyribo nucleic acid (DNA) as our genetic material. The testing method is reverse transcription polymerase chain reaction (RT PCR), a powerful technique that can be done in authorized facilities. The instruments and reagents are expensive, need trained personnel for testing (not like a simple strip that tells whether you are infected or not). In some countries, such detection facilities are rarely posing a delay in detection. An oversimplified version of detection strategy is shown above. Swab samples from respiratory canals of the suspected are taken for isolating the viral RNA genetic material. In simple terms, first we need to convert the RNA in to DNA and then run a reaction to amplify a specific fragment of our interest, that is found in the viral genetic material. It is so sensitive that a few copies of viral genetic material are enough for detection. We know the complete sequence of this virus; hence we can amplify specific regions of the virus’s genetic material first converting it into DNA. This test can be made very specific/stringent by designing a region that is very specific to the SARS CoV2.
How many are infected?
In many countries prescreened patients are subjected to testing, hence what we see is the tip of an iceberg. Once this fever season subsides, a follow up study is warranted on the population to understand how many actually got infected by SARS CoV2. RT PCR based fingerprinting is not useful there, but an antibody-based ELISA will be (such detection kits are reported already). Because an infected body retains antibodies against this virus as a memory for a longer time, even if there are no SARS CoV2 present in the body (a defence mechanism to fight against the same virus on a second attack). Many of the mild cases are unnoticed, or not considered for testing now in the middle of this pandemic season- but will be detected at a later time with this serological (blood analysis) ELISA test. It is important to know more about this virus outbreak and important to prepare more for a future pandemic.
Comparison with other Coronaviruses
SARS outbreak that happened in China (2003) and MERS in Middle East was caused by the same class of virus (Corona). A comparison between SARS CoV2 and these coronaviruses was made by Prof. Akiko Iwasaki (@VirusesImmunity). The case-fatality ratio for SARS is 9.6-11%, while that of MERS is 34.4%. SARS CoV2 virus is novel to Science, hence we are on the learning curve. With the current studies, this virus is showing a range of 2-8% case fatality ratio (based on the reported numbers). Note, this varies among different countries, among different age groups. It is difficult to predict the features of an ongoing novel viral infection (the number of the infected cases are not accurate).
No! it is not just a ´bit more than flu´!
For seasonal flu, the fatality rate is approx. 0.1%, and it is several folds higher than flu (at least 10 times, we don’t know the real number yet). The vaccine is prepared every year for flu. COVID-19 is a respiratory illness leading to pneumonia. Flu can also cause secondary respiratory infections, in absence of proper care. We know much about the influenza virus that helps us to fight against it, while we know very little about this novel CoV.
At beginning of this outbreak, many were making case fatality ratio comparisons with 1918 flu pandemic, to state the less aggressiveness of COVID-19. This is like comparing watermelons with oranges. We are comparing a century old pandemic episode with a pandemic in 2020. In 1918 the world was crippled by the WW1. Science was not that advanced; it took another 10 more years to discover Penicillin (Alexander Fleming discovered Penicillin in 1928). We did not know much about the viruses at that time. In this current era, even with much Scientific advances, this string of RNA is bringing the whole world to it´s knees.
The horse is out of the barn!
WHO was giving alarm bells and instructions at the beginning of this year about the seriousness of this pandemic, importance of testing, travel restrictions, precise quarantine, preparing a health system etc. Some countries took it more seriously than others and are now back on track. Locking down always causes economic turmoil and some countries don’t have the luxury to lockdown for several weeks! WHO praised China’s efforts to contain the transmission in Wuhan, though many countries first considered lockdown as a Draconian measure, were later forced to endorse such measures.
Flattening the curve
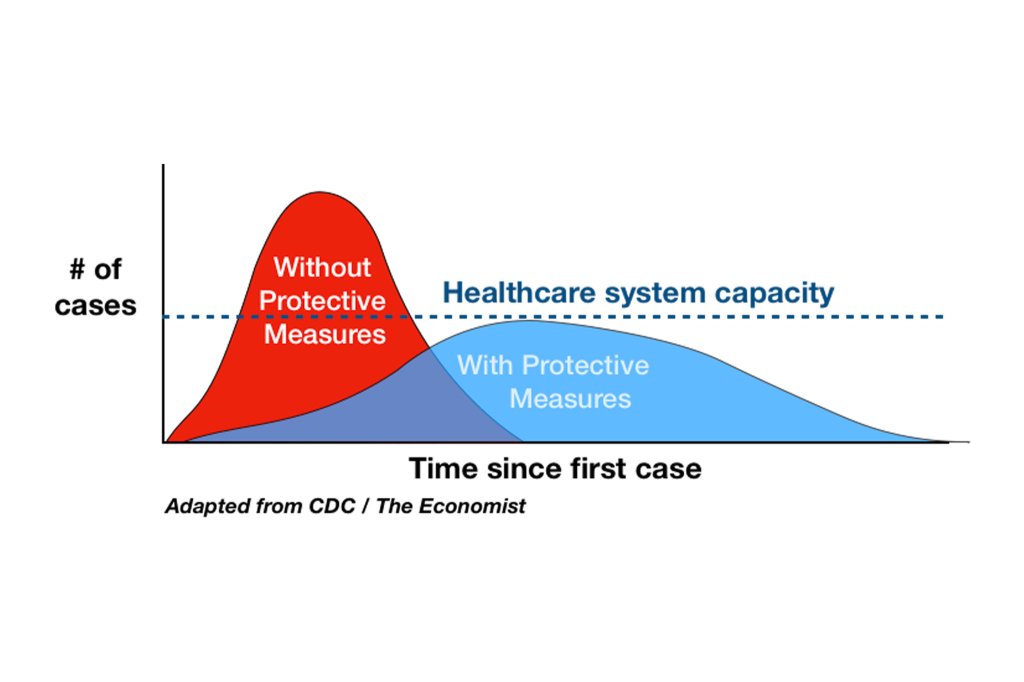
This is the graph that was widely discussed in media which says protective measures will flatten the curve (note the dotted line is the healthcare capacity). Protective measures will buy us more time to take care seriously-infected patients without choking the health system. With no such protective measures, the peak will overwhelm the health systems and more deaths will be the result. It is intriguing, that why the authorities in many countries did not take strict protective actions first? Many countries had almost 2 months of ´golden time´ to study and prepare, after the outside world knew about the outbreak in China. The horse is out of the barn, this invisible enemy does not respect borders and almost all the countries are inoculated with this virus now. Many countries are implementing strict regulations that their citizens never experienced so far!
Locking down, social distancing and catch-22
A report from Ferguson, N., M., et al (Imperial college, London) changed the mind of many leaders and forced them to take the social distancing, lockdown model as the norm, which worked in many countries including the epicenter Wuhan province, China. Social distancing is necessary to flatten the curve, will give time to the health system to breath, but will result in slowing down natural immunity. Even if many of us escape from this ´first wave of SARS CoV2´, this is going to be around for several months- or may appear next season as a variant strain (like flu coming every year), though experts predicts less probability for such a mutant. Later there may be clusters of cases since complete isolation is literally impossible in this open world. We should still practice some travel restrictions, social distancing, hygiene measures, until there is a vaccine or an anti-viral drug.
Herd immunity
Herd immunity is the process by which a majority of the population gets immunity by natural infection or vaccination thereby preventing further transmission. This is usually heard in the context of vaccination- you don’t have to vaccinate every single person, but vaccination of significant population will check the disease from spreading (the percentage population to be immunised varies depending on the nature of the virus). Note, the measles outbreak happened recently in some places where anti-vaxers refused to give vaccination to their kids.
With herd immunity strategy in mind, some countries initially prepared to gamble with this new virus but later dropped their plans. Herd immunity is not about the creation of naturally immunised ´leftover population´ when the vulnerable are dead. There will be unseen issues on experimenting with a novel virus; such as time to infect the majority of the population, medical system can get overloaded during the peak time of infections and moreover at the cost of many valuable lives. Also, if the virus mutates significantly, it can evade the immune system then the herd immunity will be a failure (though chances for such a mutation are rare).
Silent carriers
Virus spread is substantially undetected, and it is flying below the radar due to the silent carriers. These ´silent carriers´ can spread the illness, and they outnumber the detected cases, hence will be difficult to contain. It will also spread globally and may become the fifth endemic coronavirus within the human population according to a recent study.
How long SARS CoV2 virus can stay outside?
COVID-19 is a droplet disease, this virus is viable in the droplets that get out when an infected person sneezes or coughs. The droplets can travel a short distance before it falls down on surfaces. Once outside the host, viability of the viruses depends on environmental conditions. A study came out recently, analyzed stability of SARS CoV2 in aerosols and different everyday surfaces. In laboratory conditions this virus can stay stable for upto 3 days on plastic surfaces, upto 2 days on steel and a day on cardboard surfaces. Interestingly, SARS CoV2 was viable upto 3 hrs in aerosols (but infectivity depends on the inoculum shed).
Disinfectants
Soap is the best and cheapest way to get rid of this virus. This nanoscale virus has a greasy membrane coat that they take from the host cell while budding off. This lipid membrane will be easily destroyed by approx. 20 seconds washing with a good soap. Bleach is good for cleaning hard surfaces, while 70% alcohol containing disinfectant is very handy.
Origin and Conspiracy theories
With any new diseases, conspiracy theories also fly around. Most popular one was, the bioweapon theory. The coincidence presence of a high safety level virus research lab at the epicenter of this outbreak and the presence of some researchers with previous CoV research experiences at that lab fuelled these theories. Conversely, Chinese argued bioweapon testing on them by their enemies. A non-peer reviewed preprint on bioinformatic analyses on the SARS CoV2 sequence appeared (disappeared later) and claimed sequence similarities of bits and pieces of this virus with HIV and proposed the possibility of a genetically engineered virus. While these conspiracy theories were flourishing in social media, a scientific article came out very quickly in journal Nature Medicine that suggested the high sequence similarity of SARS CoV2 with bat CoV, proposing the possibility that this CoV may be transmitted from bat through an intermediate host. Their data supported the possibility that SARS CoV is a natural mutant from bats or through an intermediate host and debunked the ´designed virus´ hypothesis. Pangolins were the suspected intermediate species because of the high sequence similarity to the receptor binding region in spikes (comparison between SARS CoV2 and Pangolin CoV). Further analyses of the full virus sequence is not supportive to the hypothesis (active research is going on this field to find the real intermediate host, to prevent further interspecies transmission). Note, CoV for SARS and MERS were also originated from bats through Civet cats and Camels as intermediate hosts respectively. In the recent past, Ebola reported first from African continent, MERS from Middle East, Nipah outbreaks were reported first from Malaysia and later from Indian subcontinent. Nature is carrying out high-throughput mutation experiments on these viruses in different species and our technology to manipulate the genetics of viruses is very modest so far, compared to Nature´s approach. When other animals including us come in close contact with nature´s viral reactors, some of the mutated viruses may find a new host causing serious illness. Such zoonotic diseases (diseases that are transmitted from animals to humans) will happen in future also.
Recombinant viral vectors- viruses can be our friends too
We can create specific mutations on viruses’ genetic material or even introduce specific genes. Recently we have the technology do that for curing many genetic diseases (viruses as gene therapy vehicles). One can use molecular engineering tools to create safe recombinant viruses (viral vectors). Recombinant viral vectors are created from cells in a dish from viral genes. Cloning of essential genes into viruses and recovering safe viral tools is possible, which are utilized in research and currently in clinics too. Note, nowadays engineered safe viral vectors are used as ´cargo vans´ for delivering correct copies of a faulty gene to cure many genetic diseases.
Desperate times, desperate measures!
During this fever season, anything that has a keyword COVID-19 or SARS CoV2 gets huge attention. Many non-peer reviewed data, nowadays submitted in repositories like BioRxiv, MedRxiv get immediate attention, social media takes it, interpret in different dimensions and influence the policies of states, even that of WHO.
WHO suggested the use of Paracetamol over Ibuprofen, in case of fever during this season. This is because of a non-peer reviewed piece in Lancet, that suggested an increase in the receptor ACE2 (that is the receptor for the spikes on Corona virus) upon Ibuprofen treatment. Note, there is no strong evidence to support this. This became a topic of discussion since a French minister tweeted about this.
Old weapons in our arsenal
Remdesivir, Chloroquine/Azithromycin, Vaccines.
We are desperately trying all the weapons in our arsenal. This is a fishing experiment in the context of a new disease, a reasonable approach to bypass many stringent tedious protocols since most of these drugs are clinically approved and side effects are well documented.
One among these is a malaria drug Hydroxychloroquine/Chloroquine usage against COVID19. There are some ´preliminary data´ on its effect (with main criticism on less sample numbers) currently WHO is conducting a megatrial to confirm its effect. Chloroquine is shown to have effects on the RNA virus replication. Further, it blocks a pathway that helps the virus to enter and release its content into the infected cell. Another study suggests that this drug can act as a Zinc gate which will interfere with the RNA polymerase thereby inhibiting viral replication. Azithromycin (antibiotics) in combo with Chloroquine was administered against bacterial superinfection during Pneumonia.
Remdesivir is another promising drug candidate. It was designed for the Ebola treatment and there are some promising studies in that context. Ebola virus also uses a similar mechanism to replicate inside the infected cell, this drug will act on the RNA polymerase (which is the key protein for the viral replication) and stall it. SARS CoV2 also has RNA polymerase, hence the drug might work effectively to inhibit its function. WHO is on megatrial with this drug, along with 3 other antiviral drug combos.
Vaccine takes time. It took almost 20 months to develop the vaccine against SARS 2003. You cannot simply inject a new vaccine bypassing the strict protocols (complications from an understudied vaccine may be more damaging than this disease). Nowadays creating a vaccine or new drug may not take that much time, but the clinical trials and getting these cures into the pharmacy shelves may still take months. The virus may not wait that long, may do the damage to the vulnerable by that time. Some companies claim discovery of fragment of viral RNA as vaccine for COVID-19, but experts say that it is too early as sharpening the scalpel before the surgery. They found a fragment of RNA which may be a potential vaccine candidate for this illness. Detecting a specific region (protein or RNA) in this virus as an antigen to produce antibody in our body, that specifically recognises the virus without interfering endogenous molecules is a humongous task. This requires rigorous testings, first in lab models and animals, and eventually in people. As mentioned earlier, Corona viruses like other RNA viruses, contain single strands of RNA which mutates, and vaccines may be warranted every season, like the flu vaccine (flu virus mutates extensively). Ebola vaccine development was expensive, now resting on shelves since outbreak ended, a reason why many companies are not interested in R&D and developing vaccines ahead.
Ever-evolving viruses
RNA being the genetic material of SARS CoV2, while making copies inside the host cell there will be several errors, the reason why there are many mutations during transmissions. Also SARS CoV2 is the largest RNA virus known, with nearly 30,000 bases. RNA dependent RNA polymerase, the enzyme that makes copies of RNA does not have efficient proofreading mechanism like DNA coping system, our cells hold. This virus mutates and accumulate variations during the process of transmission from one infected individual to another. Every transmission may accumulate mutations, in general, these random mutations won’t change the virus much. SARS CoV2 virus is already quite successful in propagation. Some of such random mutations can make it more efficient, though experts like Dr. Trevor Bedford (@trvrb) predicts it may take several years to see a major drift. Flu virus which is a fragmented RNA virus, notorious for frequent mutations, escapes our immune surveillance system and that is the reason why every year we need different flu vaccine. Compared to flu virus the ´copier machine´ for SARS CoV2 is less error prone, hence natural immunity that a survivor attains by infection may help us at least for couple of seasons.
These copying errors made by the virus (that makes a new strain) are useful for genetic ´Sherlock Holmes´ researchers, since they can trace the tracks of the viral propagation. It is very important during an epidemic episode to understand more about the route-map of pathogen. For example, in US they identified viral genome from the ‘patient zero’ in Washington state who travelled from China and created a virulent cluster of cases in King county. By genomic analyses multiple transmissions from this patient zero was traced even in different states.
Don’t underestimate the power of mutations- evolution works through mutations. To understand that, here is a great experiment done on antibiotic resistance by bacteria (see the video below). The resistance is achieved by some random mutations first in a bacterium at the antibiotic boundary, which then creates a resistant colony. Then it easily grows in antibiotic medium until it reaches the higher concentration antibiotic boundary. Again it mutates/evolves to survive in the highest antibiotic concentration. Thus random mutations help bacteria to grow eventually at the highest concentration in a short time period!
Now why is it relevant in this COVID19 scenario. SARS CoV2 also undergoes random mutation and get selected depending on the environment. SARS CoV2 is a result of variation that happened in a bat or an intermediate host sometime ago. Such mutations happen in each and every infected one. When it transmits from one host to another the virus carries some of the mutations, the reason why different new strains appear. There won’t be drastic variations because more likely those variations may make virus inactive. This virus is already so successful in its transmission, managed to spread nearly 200 countries in a short time. Under a selection pressure, the virus may mutate into a strain with variations in spike protein, thereby can evade the immune system of a survivor or immunised individual-which may be a concern for future.
Kindly go through the second blog ´Briefings on the hidden enemy´ where updated research on the disease are discussed.
References
SARS CoV2
https://asm.org/Articles/2020/January/2019-Novel-Coronavirus-2019-nCoV-Update-Uncoating
https://www.nature.com/articles/s41579-018-0118-9
ACE2 Receptor and TMPRSS2
Hoffman, M et al 2020. https://www.sciencedirect.com/science/article/pii/S0092867420302294
Stability of virus on aerosols and surfaces
https://www.nejm.org/doi/pdf/10.1056/NEJMc2004973?articleTools=true
Ibuprofen and ACE2 receptor
Fang, L. 2020. https://www.thelancet.com/pdfs/journals/lanres/PIIS2213-2600(20)30116-8.pdf
Remdesivir
https://www.nih.gov/news-events/news-releases/nih-clinical-trial-remdesivir-treat-covid-19-begins
Hydroxychloroquine
https://www.sciencedirect.com/science/article/pii/S0924857920300996
Solidarity Megatrial
SARS CoV2 Genome sequencing
https://www.sciencemag.org/news/2020/01/mining-coronavirus-genomes-clues-outbreak-s-origins
https://www.nature.com/articles/s41591-020-0820-9
Blood test for COVID19
Gene therapy and viruses as delivery vehicles
https://www.nature.com/articles/d41587-019-00015-6
Origin and Conspiracy theories
https://www.nature.com/articles/s41591-020-0820-9
Pangolins may not be the intermediate host
https://www.nature.com/articles/d41586-020-00548-w
Silent carriers
https://science.sciencemag.org/content/early/2020/03/13/science.abb3221
